MALARIA PREVENTION
Welcome to the Malaria section of the Washington Travel Clinic website. This page contains valuable information on malaria and its prevention, and links to the CDC pages where you can learn about country-specific recommendations for prophylaxis.
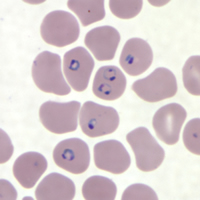
Blood smear showing malaria parasites inside red blood cells
Malaria is a serious and sometimes fatal disease; that is why travelers should assess their risk of contracting malaria before visiting areas where the disease occurs. Medicines for malaria prevention are prescribed at the Washington Travel Clinic.
For an easy online appointment to visit our clinic, please click here. Also visit our Homepage for more information about the full spectrum of our services.
Malaria Prevention
Every year, millions of US residents travel to countries where malaria is present. About 1,500 cases of are diagnosed in the United States annually, mostly in returned travelers.
Before traveling, travelers should obtain a detailed itinerary including all possible destinations and check to see if malaria transmission occurs in these locations. The CDC’s Malaria Information by Country Table provides detailed information about the specific parts of countries where malaria transmission does or does not occur. It also provides additional information including the species of malaria that occur there, the presence of drug resistance, and the specific medicines that CDC recommends for use for prevention in each country where malaria transmission occurs. Another way of finding this information is through the CDC’s Malaria Map Application. This web-based tool is particularly useful for obtaining information about transmission in specific parts of countries.
There is currently no vaccine against malaria available in the US. Prevention is achieved by taking pills before, during, and after the stay in the risk zone. Prevention involves a balance between ensuring that all people who will be at risk of infection use the appropriate preventive measures while preventing adverse effects of those interventions among people using them unnecessarily. An individual risk assessment should be conducted for every traveler, taking into account not only the destination country, but also the detailed itinerary, including specific cities, types of accommodation, season, and style of travel. In addition, conditions such as pregnancy or the presence of antimalarial drug resistance at the destination may modify the risk assessment. Click here to read more about risk assessment.
Based on the risk assessment, specific prevention interventions should be used by the traveler: malaria pills; insect repellent; long-sleeved clothing; bednets; flying insect spray; and air-conditioned or screened quarters. Click here to read more on preventing mosquito bites while traveling.
If malaria prevention medicines will be needed for the traveler, there are multiple options available. Factors to consider are the traveler’s medical conditions, medications being taken, the cost of the medicines, the potential side effects, and the convenience of the dosing schedule.
In some countries, drugs may be sold that are counterfeit or substandard. Such drugs may not be effective. Antimalarial drugs should always be purchased before traveling overseas.
About Malaria
Malaria is a serious and sometimes fatal disease caused by a parasite called Plasmodium. The parasite infects a certain type of mosquito called Anopheles, which injects the parasite into the bloodstream when it feeds on humans.
Infection with the parasites may result in a wide variety of symptoms, ranging from absent or very mild symptoms to severe disease and even death. In general, the disease is curable if diagnosed and treated promptly and correctly. In countries where cases are infrequent, these symptoms may be attributed to a cold or other common infections. Conversely, in countries where the disease is frequent, residents often recognize the symptoms as malaria and treat themselves without seeking diagnostic confirmation.
Diagnosis of malaria depends on the demonstration of parasites in the blood. The parasites can be identified by examining under the microscope a drop of the patient’s blood spread out as a “blood smear” on a microscope slide.
Antimalarial drugs taken for prophylaxis by travelers can delay the appearance of malaria symptoms by weeks or months, long after the traveler has left the malaria-endemic area, because the parasite can lay dormant in the liver. Such long delays between exposure and the development of symptoms can result in misdiagnosis or delayed diagnosis because of reduced clinical suspicion by the healthcare provider. Returned travelers should always remind their healthcare providers of any travel during the past 12 months in areas where malaria occurs. Patients who have recovered from the first episode of illness may suffer several additional attacks (“relapses”) after months or even years without symptoms. Relapses occur because of dormant parasites in the liver that may reactivate. Treatment to reduce the chance of such relapses is available and should follow the treatment of the first attack.
Where malaria is found depends mainly on climatic factors such as temperature, humidity, and rainfall. The disease is transmitted in tropical and subtropical areas, where Anopheles mosquitoes can survive and multiply and the parasites can complete their growth cycle in the mosquitoes. In many endemic countries, transmission does not occur in all parts of the country. Even within tropical and subtropical areas, transmission will not occur at very high altitudes, during colder seasons in some areas, in deserts (excluding the oases), and in some countries where transmission has been interrupted through successful control/elimination programs.
Generally, in warmer regions closer to the equator, transmission will be more intense and the disease is transmitted year-round. The highest transmission is found in Africa South of the Sahara and in parts of Oceania such as Papua New Guinea. In cooler regions, transmission will be less intense and more seasonal.
If symptoms of malaria occur during travel, the traveler should seek immediate medical attention. Malaria is always a serious disease and may be a deadly illness. Travelers who become ill with a fever or flu-like illness either while traveling in a malaria-risk area or after returning home (for up to 1 year) should seek immediate medical attention and should tell the physician about their travel history.
Travelers who are assessed as being at high risk of developing malaria while traveling should consider carrying a full treatment course of medicines with them. Providing this reliable supply of medicine (formerly referred to as standby or emergency self-treatment) will ensure that travelers have immediate access to appropriate and high-quality medicine if they are diagnosed with malaria while abroad. Depending on the medicine they are using for prevention, this could either be atovaquone/proguanil or artemether/lumefantrine.





